As the proportion of elderly individuals within the population grows, the incidence of hip fractures increases. Traditionally, orthopedic surgeons used to focus on surgical treatment of hip fractures; however, the field’s appreciation for the importance of postoperative rehabilitation has been increasing recently. Many studies have shown that proper rehabilitation after hip fracture surgery can shorten hospital stays and improve clinical outcomes. However, such studies use different methods and published rehabilitation protocols address varying aspects that do not always overlap. Here, we review and summarize the latest guidelines and studies on postoperative rehabilitation of elderly patients with hip fractures.
INTRODUCTION
An increase in life expectancy will lead to a concurrent increase in the proportion of elderly individuals in the population, and consequently to a rise in the incidence of hip fractures. The number of hip fractures is expected to increase to about 4.5 million per year worldwide by 2050. Even with successful surgery, the mortality and the risk of permanent disability and dependence remain high in patients with hip fractures. As a result, medical costs associated with the treatment of these patients are increasing. For these reasons, hip fractures are an increasingly important global public health issue.
Until now, orthopedic surgeons used to focus on the surgical treatment of hip fractures, with interest in postoperative treatment remaining relatively low. Proper rehabilitation after surgery has been shown to shorten hospital stays, improve physical function, and help patients maintain independent daily life, outcomes which reduce the burden of medical and caregiver expenses. Because of the high proportion of elderly patients with hip fractures, the effect of rehabilitation after hip fractures on elderly patients is greater than in younger patients. Orthopedic surgeons’ interest and participation in postoperative rehabilitation specifically designed for hip fracture patients who underwent surgery are important for proper rehabilitation planning and functional recovery of the patients. Important factors for optimizing rehabilitation plans include fracture type, localization of other injuries, and mode of fixation5). Clinical guidelines for post-hip-fracture surgery rehabilitation have been introduced in various countries, and several reports summarizing various rehabilitation methods have been published. The purpose of this article is to review and summarize the latest guidelines for rehabilitation of elderly patients with hip fractures following surgery that can be performed during hospitalization and after discharge.
REHABILITATION DURING HOSPITALIZATION
1. Early Mobilization
Early mobilization is important for optimal postoperative management of patients with hip fractures. Early mobilization includes getting in and out of bed, sit-to-stand, sit from a chair with arms, and walking with an assistive device. This initial strategy is strongly recommended in many guidelines. Weight bearing is allowed except for patients who: (i) were ordered non-weight bearing by the surgeon and (ii) were non-ambulant before fracture. Early assisted ambulation (started within 48 hours of surgery) accelerates functional recovery and is associated with more direct discharge to home and less discharge to high-level care. Mobilization on the next day after surgery, unless medically or surgically contraindicated is recommended.
2. Physical Therapy in the Acute Care Phase after Surgery
Patients on average lose more than 50% of their fractured limb muscle strength within the first postoperative weeks compared with their non-fractured limb; those with trochanteric fractures experience the greatest relative loss. Many studies support intensive physical therapy in the acute care phase on the basis of the observation that it improves recovery in comparison with delayed physical therapy (which begins more than 3 or 4 days after surgery). In addition, patients following a high-intensive physical therapy program (3 daily sessions) in the acute phase in hospital on average reached functional discharge criteria 10 days earlier than the usual physical therapy group (1 daily session). Patients from the former group reported good program compliance without sacrificing safety. However, all items in high-intensive physiotherapy programs cannot be performed in every patient in the acute phase following hip fracture surgery.
We introduce several exercises that are strongly recommended during the acute care phase after surgery. Patients can start with ankle pumps that perform dorsiflexion and plantarflexion of the ankle after surgery (Fig. 1A). Knee extension strength training of the fractured limb is feasible when started in the acute phase (Fig. 1B). Additionally, after careful assessment, the impact of a progressive fractured-limb knee-extension strength training session added once a day; with the patient seated next to the bed and use an ankle weight cuff while performing three sets of 10 repetitions with maximum load is advised. No adverse events or hip fracture–related pain will be seen, and fractured limb strength deficit will be reduced on average from 50% to 32%. Straight leg raise (Fig. 1C) follows the exercises mentioned above. The goal of these exercises is to increase muscle strength and gain control of the limb, especially gluteal and quadriceps muscles. Yet, it is necessary to consult with the orthopedic surgeon who performed the surgery on whether such physical therapy can be performed.
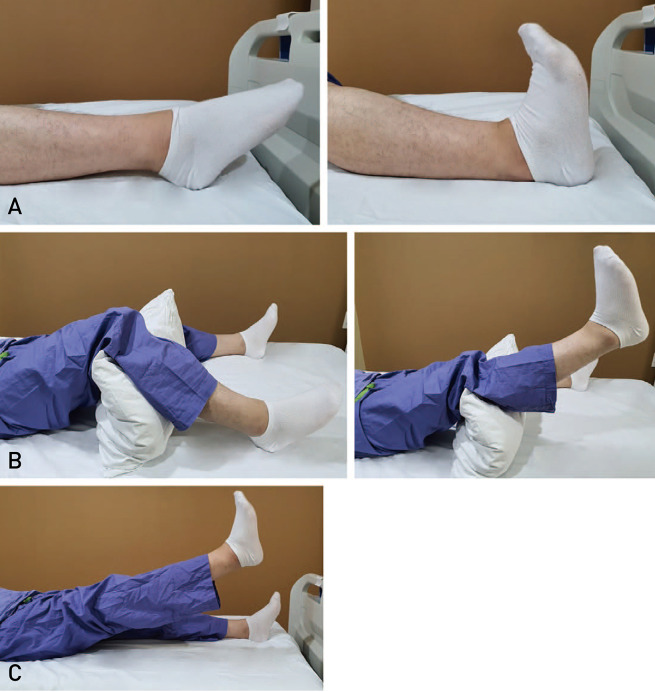
Fig. 1
(A) Ankle pumps. Ankle plantar flexion (left) and ankle dorsiflexion (right). (B) Knee-extension strength training. While supine, the patient tightens quadriceps in an attempt to straighten the knee (hold for 5–10 seconds). (C) Straight leg raise. While supine, the patient tightens the quadriceps, flexes the hip and keeps the knee straight while lifting the extremity off the bed (hold for 5–10 seconds), then lowers it slowly.
3. Score Monitoring during the Acute Care Phase
The primary goal of postoperative rehabilitation is to help patients return to their pre-fracture status; therefore, quantification of preoperative and postoperative scores is needed to objectively assess recovery. Measuring preoperative activity scores and comparing them to postoperative follow-up values can help predict functional outcomes of postoperative rehabilitation. These scores can be continuously monitored in discharged patients. Several useful scoring systems for monitoring during the acute care phase are available.
The cumulated ambulation score, which can be used for patients with hip fractures, was specifically developed to plan and monitor progress of activities during a daily acute hospital physiotherapy program. This system can quantify basic mobility information; it focuses on pre-fracture basic mobility and is designed to be used every day postsurgery from the beginning of rehabilitation until independence in basic mobility is reached or until discharge. The modified new mobility score (NMS) focuses on pre-fracture functional levels. This score is easily applicable and provides the ward personal with a prediction of mortality and rehabilitation outcome. The NMS can be measured immediately after hospitalization to assess the pre-fracture status and then during outpatient follow-up after discharge. The timed up and go (TUG) test generates a score that measures functional mobility using the time (in seconds) that it takes an individual to rise from an armchair, walk 3 m to a line drawn on the floor and return to the chair. The test has been used worldwide in many studies and is useful for predicting the results of rehabilitation through the quantification of functional mobility. In particular, it is possible to predict the possibility of falls. However, patients who are not allowed full weight bearing postoperatively and patients with no pre-fracture indoor walking ability (walking aids allowed, but without assistance) cannot be tested. TUG test is performed the day before the patient is discharged and can be additionally performed after follow-up in the outpatient settings. The verbal rating scale (VRS), also known as verbal pain scores is a powerful tool used to assess pain experience. The VRS focuses on hip fracture-related pain at all time-points following fracture. Unlike the visual analogue scale, which has been associated with high error rates when used in elderly patients, the VRS has been found to have low error rates. These scoring systems provide good tools for assessing pre-fracture status and for continuous assessment of postoperative clinical outcomes.
Table 1
| Monitoring score | Characteristic | Measurement method |
|---|---|---|
| Cumulated ambulation score | Basic mobility at pre-fracture, to daily post-surgery use until independence in basic mobility is reached. | 1) Getting in and out of bed |
| Early prediction of short-term postoperative outcome after hip fracture surgery (length of hospitalization, 30-day mortality). | 2) Sit to stand to sit from a chair with arms | |
| 3) Walking with an appropriate aid (0: not able to, 1: able to with assistance from one or more persons, 2: independent of human assistance) | ||
| Total score from 0 to 6 | ||
| Modified new mobility score | Functional level at pre-fracture and follow-up. | 1) Indoor walking |
| Valid predictor of mortality and rehabilitation outcome. | 2) Outdoor walking | |
| High inter-tester reliability. | 3) Shopping- It provides a score between 0 and 3 for each (0: not at all, 1: with help from another person, 2: with an aid, 3: no difficulty) | |
| Total score from 0 to 9 | ||
| Timed up and go test | Score system that measures functional mobility for quantification of the mobility level. | Time from seated in a chair with arms, walk 3 meters to a line drawn on the floor, turn around, walk back, and sit down. |
| The time is prolonged if a standard 4-legged walker is used. | ||
| Verbal rating scale | Hip fracture-related pain at all time-points following fracture. | 0: no pain, 1: slight pain, 2: moderate pain, 3: severe pain, 4: unbearable |
| Low error rates compared with graphic instruments like the visual analogue scale among the elderly. |
4. Multidisciplinary Management
Recently, the comprehensive multidisciplinary management approach has become a cornerstone of rehabilitation programs. Interdisciplinary teams systematically evaluate elderly patients with the goal of assessing and optimizing medical, psychosocial, and physical capacities, including plans for early discharge. Because most hip fractures occur in elderly patients, a multidisciplinary rehabilitation strategy involving geriatricians and other specialists is important. To ensure best outcomes, this management should start immediately when the patient is hospitalized and continue during patient’s rehabilitation after discharge. NICE and ANZ guidelines both recommend orthogeriatric assessment and rapid optimization of fitness for surgery. Early identification of individual goals for multidisciplinary rehabilitation is important; these goals include recovery of mobility and independence, and facilitation of the return to pre-fracture residence and long-term wellbeing. Integration with related services, particularly mental health, fall prevention, and bone health services, should be considered. The orthopedic surgeon should particularly focus on: (i) postoperative mental health care including postoperative delirium, (ii) fall prevention management (such falls can be associated with postoperative delirium), and (iii) osteoporosis management.
In a recent prospective cohort study, multidisciplinary management for elderly patients with hip fractures enhanced functional recovery, prevented secondary fractures and reduced the cost of hip fracture care, and thus relieved the financial burden on society. Nordström et al. noted that multidisciplinary management significantly increases physical function and mobility in comparison with conventional care in patients with hip fractures; however, it does not affect the chance of being discharged to one’s own home or survival.
REHABILITATION AFTER DISCHARGE
1. Physical Therapy after Discharge
In many patients with hip fractures, gait and balance functions recover in the first 6–9 months after surgery. During this period, most patients are discharged from the hospital and live at home (with out-patient follow-up) or in nursing facilities. In the subacute period after surgery, physical therapy focuses on enhancing safe mobility and improving muscle function.
Lee et al. conducted a meta-analysis to assess the impact of progressive resistance exercise after hip fracture surgery. Progressive resistance exercises resulted in greater improvements in the overall mobility of patients than in the control groups, and specifically in mobility related to activities of daily living, balance, and lower-limb strength. Progressive resistance exercises used in rehabilitation programs typically include knee flexion/extension, lunge, leg press, hip abduction, and hip extension. Exercise intensity, number of repetitions per set, and number of sets vary from study to study, and exercise items vary in some details. However, Lee et al. did mention small cohorts, variable outcomes, and heterogeneity of follow-up periods as limitations. Therefore, there is a need for large-scale randomized control trials to better quantify the effects of exercise programs to facilitate reaching a consensus. During the bone-healing stage (6 months to 2 years) at the fracture site, more attention to increasing the intensity of physiotherapy and other exercises (e.g., balance, functional activities, endurance) is needed in addition to progressive resistance training.
2. Supervised Home-based Exercise Therapy
The effectiveness of supervised home-based exercise therapy is another key issue in post-hip fracture rehabilitation programs. Latham et al. used programs that instructed patients to perform home exercise routines several times per week for several months. Physical therapists visited the home and taught the patient relevant rehabilitation exercises, and also provided monthly telephone calls. DVD versions of these programs were also provided to participants. 33) Many studies hypothesized that home-based exercises would be superior to standard care; however, the results are controversial. Two recently meta-analyses came to different conclusions about these programs. Kuijlaars et al. 34) noted that there was no evidence to support the benefit of home-based exercise therapy after hip fracture for most functional outcomes and activities. On the other hand, Wu et al. 35) reported that home-based rehabilitation has considerable positive effects on physical functioning after hip fractures. The latter meta-analysis included more recent studies than the former one; however, it is unclear which meta-analysis is more reliable because the methods and outcome measurements differed. Therefore, additional studies of the potential benefit of home-based exercise are warranted.
REHABILITATION OF PATIENTS WITH COGNITIVE IMPAIRMENT
Recovery following a hip fracture tends to be particularly challenging for patients with cognitive impairment. Approximately 19% of all elderly individuals with hip fractures have dementia, and up to 40% of them with a hip fracture have some form of cognitive impairment (e.g., dementia, delirium, mild cognitive impairment). Rösler et al. introduced a specialized geriatric ward called the cognitive geriatric unit (CGU) for patients with hip fractures and dementia. The CGU has additional components in comparison with conventional geriatric treatment (e.g., hidden exit doors, increased light in hallways and patient rooms, night lights, a treatment room on the ward) to decrease patient transferal. Bellelli et al. used body weight–supported treadmill walking for postoperative rehabilitation of an elderly woman with severe cognitive impairment who underwent surgery after a hip fracture. Manual assistance was provided to this patient to help her maintain upright posture and a normal gait pattern. Treadmill walking was done daily with a daily increase in the length of exercise, which reached 40 minutes by the time of discharge 39). Although the current evidence is derived from a small number of studies with quality limitations, it should be noted that it is feasible to implement rehabilitation programs focused on individuals with cognitive impairment. The barriers to more advanced studies on these patients include: (i) the absence of a consensus on components that should be included in the rehabilitative programs, (ii) the absence of a uniform approach to determining how to engage this group during rehabilitation, (iii) the lack of uniformity in assessing cognitive impairment, and (iv) differentiating cognitive impairment from delirium and depression.
CONCLUSION
Postoperative rehabilitation may improve postoperative clinical results and quality of life in hip fracture patients; however, because of the diversity of research methods and differences in the results among published studies, there is insufficient data to conclusively substantiate this potential benefit. It is crucial for an orthopedic surgeon to advocate for patient-specific rehabilitation approaches and understand the potential strengths and weaknesses of different options.





 Health Corp LLP
Health Corp LLP